Time is testicle!
Scrotal EDE is one of the topics that Greg presents at EDE 3. While not a life-threatening entity (try telling that to an 18 y.o. male!), it still carries with it significant morbidity. Ultrasound is key to the diagnosis and can help assess the success of attempts at de-torsion.
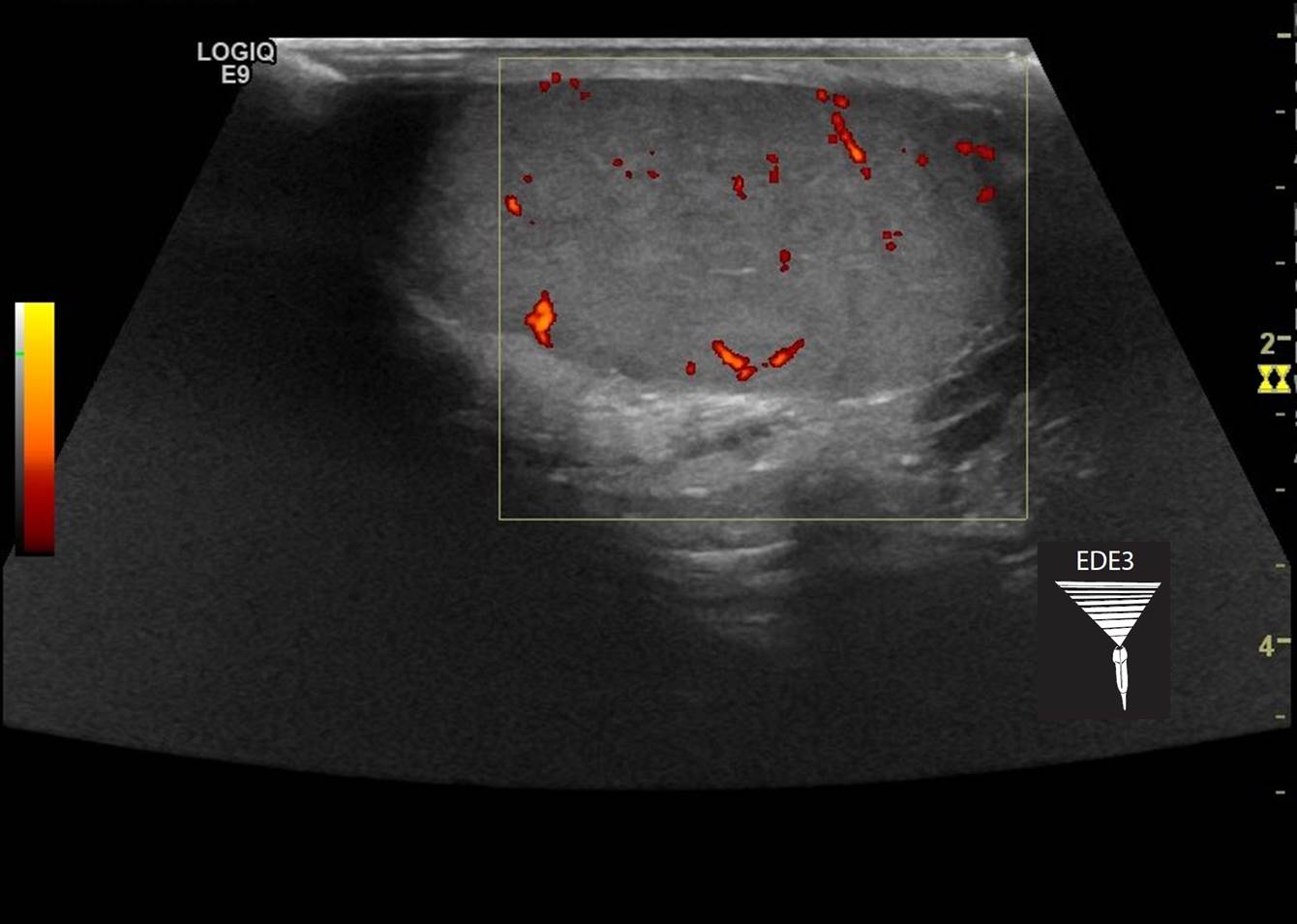
I recently saw an 18 y.o. male with scrotal pain at a small 20-bed hospital one hour from Sudbury where I work once a month. The pain had started suddenly 6 hours prior to arrival. He had 2-3 milder episodes over the last few months. The triage nurse alerted me to the patient. Unfortunately, the bedside ultrasound machine in their department does not have color Doppler. Rats! The ultrasound department was within one hour of closing and, of course, it was a Friday. So we whisked him over to ultrasound before they closed, and before my H&P. Although the ultrasound tech is very experienced, I quickly reviewed technique with her. I find that some ultrasound departments do not always use power Doppler as opposed to simple color Doppler. She was planning on using power Doppler but she wasn’t aware of the whirlpool sign. I quickly explained it to her and she found some images online. The first image is the affected testicle. The 2nd image is the unaffected side.
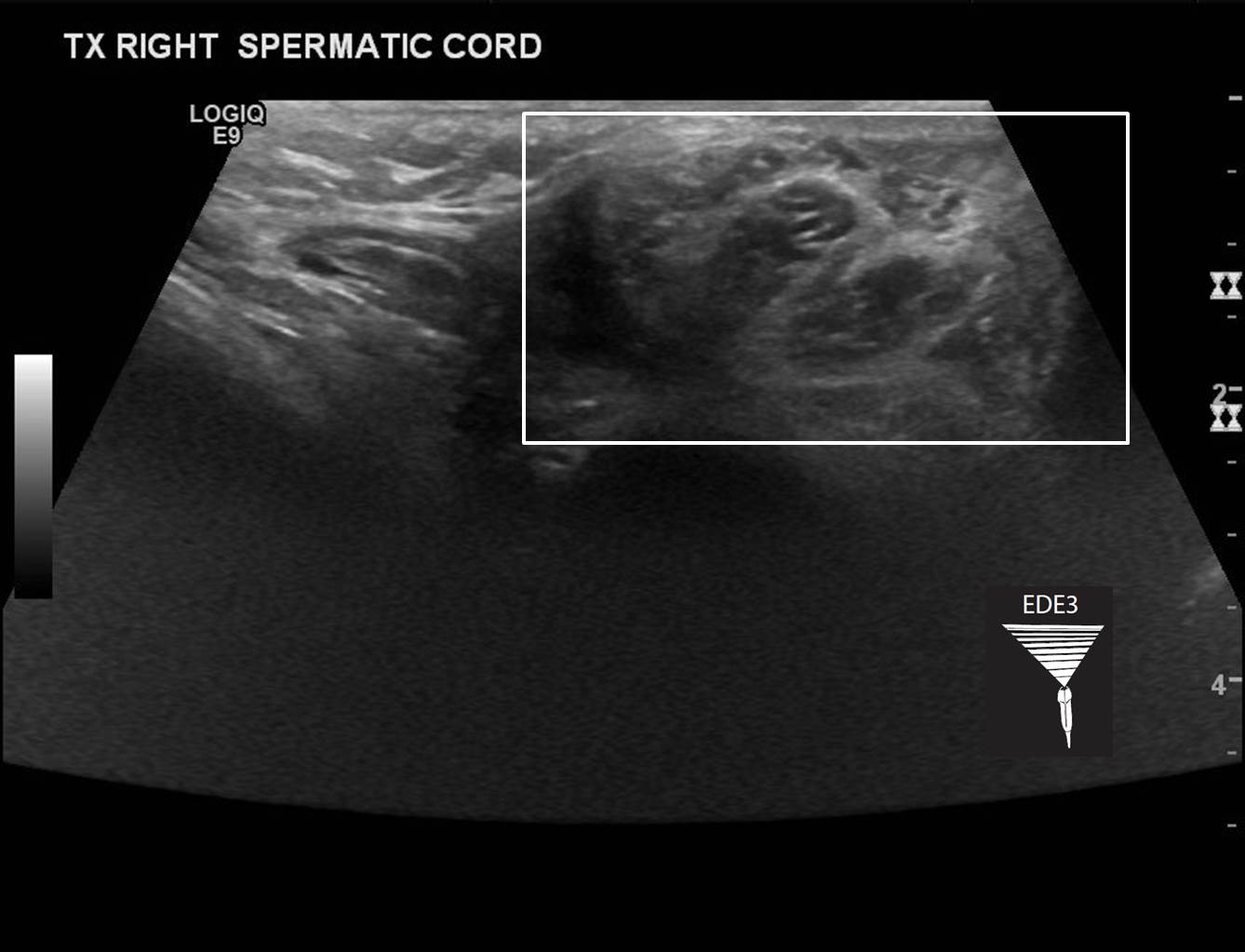
So, no flow in the right testicle and normal flow on the left. There is also a hydrocele on the right and the head of the epididymis looks large. The box in the image below shows the cord bunched up and layered on itself. Not quite a whirlpool sign, but the idea is the same.
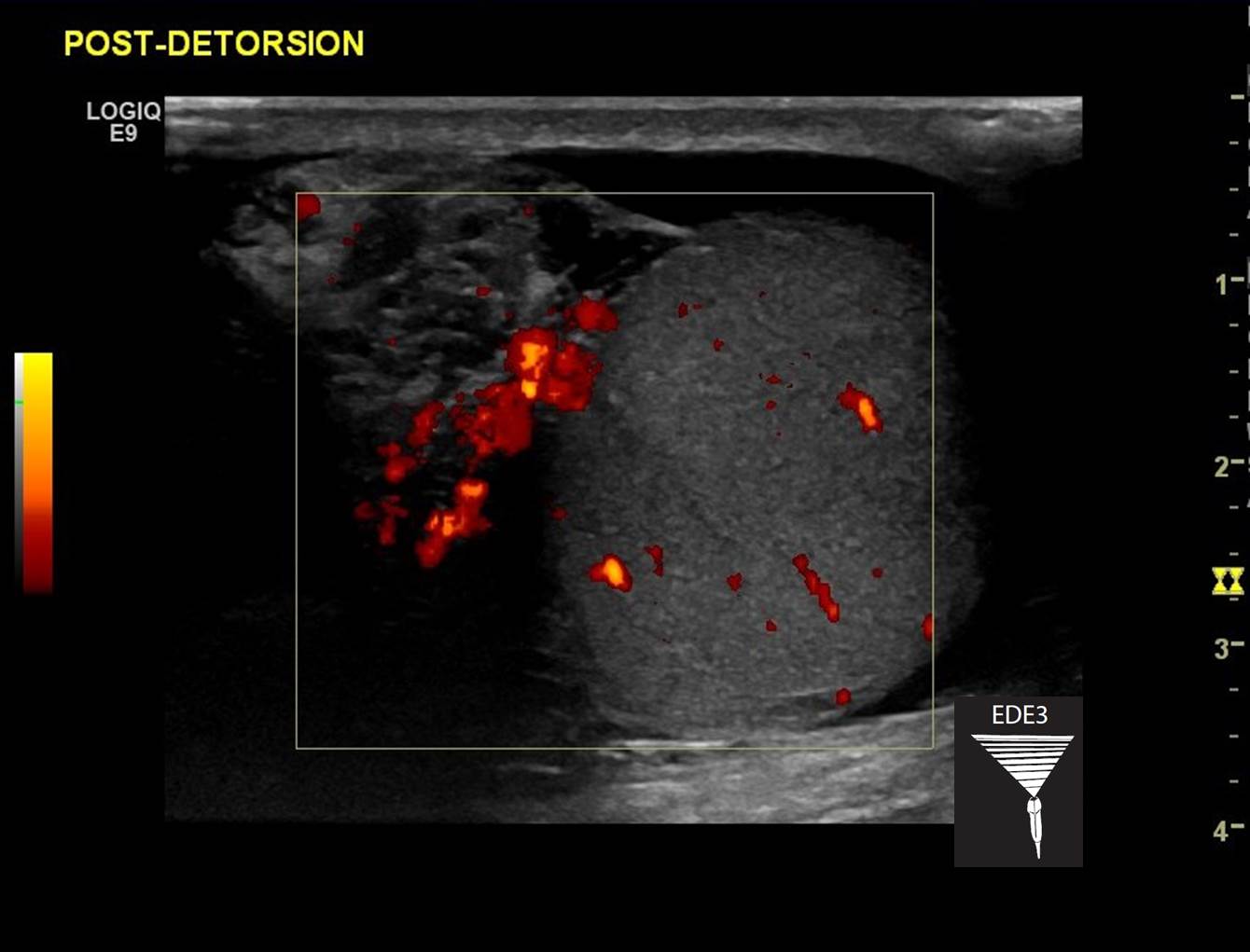
After the initial ultrasound, we brought him back to the ED, placed an IV and gave him some fentanyl. Given that he was likely 3 hours from being in the OR, an attempt at detorsion was made. The fentanyl was so effective that it was hard to know if his pain improved with the detorsion attempt. A follow-up ultrasound comfirmed that flow had returned (see image below). This was invaluable. External rotation was performed because most testicles tort by rotating internally. But a significant minority (up to 40%) will twist in the other direction. In a case like this, the only way to know for sure that you rotated the testicle in the correct way would be to check flow after the attempt. If flow had not been reestablished, an attempt at internal rotation would have been warranted.
He was in the OR 3-4 hours later in Sudbury where his testicle was a bit dusky but untorted and likely to survive. Another testicle saved!
We don’t tend to use color Doppler much with EDE/POCUS. But if you’re in the market to get a new ultrasound machine or upgrade, make sure you get color Doppler. You never know when you’ll need it!







An excellent save. As a point of curiosity, I wonder if one of the Doppler probes (for foetal hearts or peripheral pulses) would do in a pinch.
Short answer is no. Venous flow goes first then capillary. Arterial pulse would be the last to go. I’m also not sure if it would be easy or hard to pick up a pulse in a normal patient with such a device since it’s such a small artery. Never tried it.